Is my vertigo from Ménière’s disease?
- Posted on: Oct 17 2015
First, let’s clarify what vertigo really means. Vertigo refers to the sensation of dizziness that is specifically described as the feeling of the room rotating in a circular manner around you. Vertigo is the name of a symptom, not the name of a disease. For example, vertigo is one of the symptoms of Ménière’s disease, but there are other symptoms that we need to look for to confirm the diagnosis. There are also many other symptoms of dizziness that cause issues with balance, but are not true vertigo. Some diagnoses such as Ménière’s disease and benign paroxysmal positional vertigo (BPPV) have to present with true vertigo to confirm the diagnosis, and other diseases can be completely ruled out if vertigo is present.
Ménière’s disease is synonymous with endolymphatic hydrops. Our vestibulocochlear apparatus, the organ of the inner ear that is in charge of our hearing and balance, has 2 fluid chambers. The chambers are separated by a very thin membrane. One chamber contains endolymph fluid, and the other contains perilymph fluid. One chamber has high sodium and low potassium concentration, and the other one has the opposite composition of low sodium and high potassium concentration. The membranes around these chambers are in charge of maintaining that delicate balance of mineral difference.
Occasionally, the pressure within the endolymphatic chamber increases to the point that the delicate membrane might rupture. If this happens, the two fluid chambers mix and the difference in the concentration of minerals is lost. The membrane usually comes back together after the rupture, and it can regenerate the difference in the concentration of sodium and potassium within a few minutes.
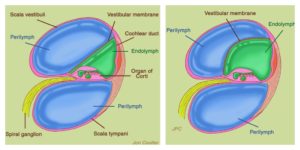
The diagram on the left shows the normal anatomy of the endolymph and perilymph chambers. The diagram on the right shows the increased pressure in the endolymph chamber before a rupture.
Each one of these ruptures corresponds to an attack of Ménière’s disease. Patients usually describe a fullness in the affected ear a few minutes before the attack. Occasionally there is also a feeling of ringing in that ear that comes before the attack happens. Physiologically, this corresponds to the increase in fluid pressure in the endolymph chamber and the stretching of the membrane before the actual rupture happens. If the pressure keeps rising, eventually the membrane ruptures. This is the actual attack of dizziness. Patients describe it as a sudden onset of severe vertigo that is not related to any positional changes or other activity. It is usually very debilitating, and patients often fall down to the ground although they are fully conscious and awake. Each attack usually goes on for 20 to 30 minutes before the vertigo is gone. Some patients also feel that the affected ear loses quite a bit of hearing during the attack. Most patients describe a sensation of lightheadedness for several hours after the attack, and the hearing is also gradually restored. This corresponds to the activity of the now resealed membrane restoring the difference in sodium and potassium concentrations in each fluid chamber.
Many patients get attacks of Ménière’s disease at unpredictable times, and they occasionally come in succession over a few days or weeks. It is believed that the sudden rise in the pressure of the endolymph is due to rise in sodium, which could correspond to sodium concentration in the rest of the body. High sodium diet as well as one-time consumption of foods high in sodium can bring the pressure up to the point of inducing an attack.
The medical work up Ménière’s disease is a diagnosis of exclusion. Most of the information we need to confirm the diagnosis is based on the history offered by the patient. Based on the history and any findings on physical exam, your ENT doctor may choose to preform some tests to rule out any other possible reasons for your vertigo attacks. If no other reasons are found, and the history is convincing, the diagnosis of Ménière’s disease can be confirmed.
The treatment for Ménière’s disease is rather straight forward and simple. First and foremost, patients are encouraged to adhere to a low salt diet. They are encouraged to lower the daily consumption of sodium, and to read labels on prepared foods. Foods that contain a high amount of sodium can suddenly raise the endolymph pressure and cause another attack. Many patients also respond nicely to diuretics (water pills) that tell our kidneys to flush away excess sodium in our urine. If a patient is going through a rough series of frequent attacks, they might also respond to anti-dizziness medications or anxiety medications, but these treatments are not recommended for the long term. Each rupture and eventual resealing of the membrane can cause scar tissue; and many patients with recurrent attacks eventually start losing more hearing in the affected ear with each subsequent attack. A few patients refractory to all medical therapy might respond to some surgical procedures designed to provide a route for decompression of the endolymph fluid, or actually cutting the nerve that goes from the inner ear to the brain. However, these surgeries are invasive and have their own side effects. The recommendation for surgery is saved for only a small selection of patients.
If you believe you are suffering from symptoms of vertigo, you should see your ENT specialist for an accurate diagnosis and management plan. A specialist can determine if you’re suffering from Ménière’s disease or possibly from other sources of dizziness that need other treatments.
Tagged with: cochlea, diuretic, dizziness, ear nose throat, endolymph, endolymphatic, ENT, Isaac Namdar, Isaac Namdar MD, meniere, meniere's, meniere's disease, New York, new york city, ny, NYC, Otolaryngology, Otorhinolaryngology, perilymph, perilymphatic, true vertigo, vertigo, vestibule
Posted in: Ears